What is gluteal tendinopathy?
Gluteal tendinopathy occurs when there is damage to the gluteal tendons over the greater trochanter. Damage can occur when there is injury due to tiny tears that may have occurred to the tendon after a period of time.
In the past, this condition has often been refered to as ‘greater trochanteric pain syndrome’ and trochanteric bursitis. Gluteal tendinopathy is also now believed to be the main cause of lateral hip pain.
Prevalence and risk factors of gluteal tendinopathy
Gluteal tendinopathy is most prevalent in women over the age of 40 years with 23.5% of women and 8.5% of men affected between the ages of 50 and 79 years old. This condition affects all individuals including those who are sedentary or athletes.
It is anticipated that the prevalence of gluteal tendinopathy will continue to increase as the society is aging and there is also increasing participation of females in sports. This condition is prevalent particularly among postmenopausal women and has a negative impact on the quality of life as it may affect sleep and activities of daily living.
What are the symptoms of gluteal tendinopathy?
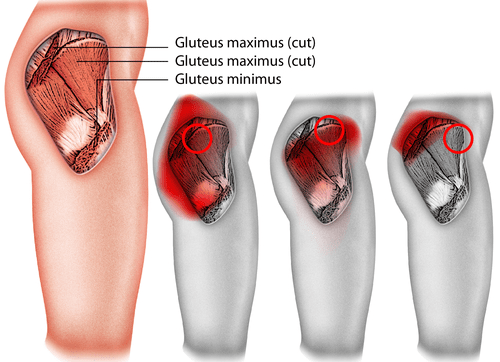
A patient with gluteal tendinopathy usually presents with pain and tenderness mainly at the area of the greater trochanter (the prominent bony area which is on the outer side of the thigh below the hip). This pain may also radiate throughout the area and sometimes down the outer side of the thigh towards the knee.
The pain normally starts gradually and worsens all the time and may be associated with changes in physical activity, during a slip or after a fall. Gluteal tendinopathy can be debilitating as it may interrupt sleep and limits the performance of daily routines.
Patients usually complain that the pain is often worst at night and aggravated when they try to sleep on their side. Other problems include pain on walking, standing on the affected leg, climbing the stairs or going uphill. Patients may also experience stiffness.
What is the diagnosis for gluteal tendinopathy?
Gluteal tendinopathy is mainly a clinical diagnosis which means that the diagnosis is achieved via patient history and physical examination of the patient. Imaging of the hip and lumbar spine may aide to rule out any other diagnosis.
Imaging may also be necessary to exclude bony or significant injury that may require surgical intervention. Findings on imaging should correlate with clinical features.
Ultrasound and magnetic resonance imaging (MRI) are the main investigations used for complaints of lateral hip pain.
MRI is considered the gold standard for assessment of gluteal tendons as it may be used to assess inflammatory changes of the surrounding areas and possible surrounding muscle atrophy.
Treatment and management of gluteal tendinopathy
The best management for gluteal tendinopathy is yet to be known. There is little evidence in the current literature that has found any effective treatment. This may be due to the uncertainty of how or why this condition develops.
Management techniques include exercise and education to manage the load on the tendon, steroid injections, and surgical interventions. Analgesics can also be used to provide adequate pain relief for the patient. Other measures such as an ice pack or hot pack may also be used if found to be helpful. Rest may be recommended to aid in pain relief.
Surgical intervention is only recommended for gluteal tendinopathy those who have failed oral medications and rehabilitation. The evidence for outcomes of surgical repair is weak as there are very limited studies that have been done.
The largest study reports that 90% of 72 patients who had surgery were pain-free or had minimal pain 12 months after surgery, and the number of patients who considered their walking to be “normal” increased from 5% to 78%. The longest follow-up after surgical tendon repair is 5 years and 16 out of 19 patients maintain the improvements gained in the first 12 months after surgery.
Gluteal tendon repairs can now be done endoscopically (surgery is done through a small incision thus increasing healing time and reducing scarring) which is less invasive and is associated with reduced postoperative infection, scarring and pain along with an accelerated rehabilitation.
Endoscopic techniques require greater surgical skill and unsuitable for larger tears or tendon detachments due to retraction of the muscle and requirement of greater visualization.
Gluteal tendinopathy occurs in both sedentary and athletic individuals; particularly in females who are over the age of 40 years old. The evidence for best management of gluteal tendinopathy is poor and the underlying mechanisms contributing to the condition is only starting to be understood. The interventions that have been reported in the current literature do little to address the possible underlying mechanism that causes the condition.
Existing treatments aim to relieve pain via medication, rehabilitation, and patient education. More studies should be done to clarify the underlying mechanism causing the condition and may eventually guide the development of better management strategies.
FAQs
Q. How long does gluteal tendinopathy take to heal?
A. There is no specific timeframe in which gluteal tendinopathy heals, as it is down to the individual to ensure all recovery steps are covered. Overall, the wait can be between 8 weeks and 52 weeks
Q. How do I sleep if I have gluteal tendinopathy?
A. Lying on your side can compress either gluteal tendons. It is recommended to sleep on the side which is not prone whilst healing takes place. Sometimes pillows have been used in certain cases to help alleviate pain.
Q. Does gluteal tendinopathy go away on its own?
A. Yes, but this can be many weeks to many months. It is important that within this period. The affected area is well rested and stretched.
SOURCES
[1] Alvarez-Nemegyei J, Canoso JJ. Evidence-based soft tissue rheumatology: Iii: Trochanteric bursitis. J Clin Rheumatol. 2004; 10(3):123-4.
[2] Segal NA, Felson DT, Torner JC et al. Greater trochanteric pain syndrome: Epidemiology and associated factors. Arch Phys Med Rehabil. 2007; 88(8):988-92
[3] Del Buono A, Papalia R, Khanduja V et al. Management of the greater trochanteric pain syndrome: A systematic review. Br Med Bull. 2012; 102:115-31.
[4] Fields KB. Running injuries – changing trends and demographics. Curr Sports Med Rep. 2011; 10(5):299-303.
[5] Lepers R, Knechtle B, Stapley PJ. Trends in triathlon performance: Effects of sex and age. Sports Med. 2013; 43(9):851-63.[/trx_infobox]